Freehold (732) 294-9393
Freehold (732) 294-9393

Cracked heels may make you want to think twice about showing off your feet in warmer weather. However, cracked heels may be harmful to more than just the appearance of your feet. If deep fissures and cracks develop in your heels, they may make walking and standing painful for you. Additionally, these openings make way for germs to enter through your skin and cause infection.
There are several different causes of cracked heels. One of the most common reasons for this ailment is dry skin. This problem may make your keeps feel rough tight and itchy. Dry skin may be caused by cold air, extremely hot water, harsh soaps, and aging. Skin disorders such as eczema and psoriasis may eventually lead to dry skin. In some cases, complications may arise from cracked heels. Some of these complications are a loss of feeling in the heel, cellulitis, or a diabetic foot ulcer.
There are ways you can try to prevent getting cracked heels. One of the best ways to do so is to avoid wearing flip flops and sandals because these shoes increase your risk of drying out your feet. You should also avoid wearing shoes with a tall skinny heel, because these shoes cause your heel to expand sideways. At night, you should slather on a thick moisturizing cream on your feet and then cover them in socks to keep your feet moisturized overnight. Drinking water to stay hydrated is also a good way to ensure that your skin doesn’t become dry.
If you suffer from a severe case of cracked feet, you should make an appointment with your podiatrist to see what treatment methods are best for you.
 People who like flip flops generally enjoy their simplicity. They are simple to slip into, and are inexpensive to purchase. Despite these types of benefits, these shoes may not be the best shoe to wear. This is for several reasons, including the fact that most flip flops offer little or no arch support, weaken the foot muscles as a result of them needing to hold the shoe on the foot, and strain the Achilles tendon. Additionally, wearing flip flops may make it easier to fall, and the toes may become bruised. It is beneficial to wear flip flops to the pool, beach, and shower areas, but your overall foot health may benefit from limiting the time that your feet spend in flip flops. If you would like more information about the dangers of wearing this type of shoe, please consult with a podiatrist.
People who like flip flops generally enjoy their simplicity. They are simple to slip into, and are inexpensive to purchase. Despite these types of benefits, these shoes may not be the best shoe to wear. This is for several reasons, including the fact that most flip flops offer little or no arch support, weaken the foot muscles as a result of them needing to hold the shoe on the foot, and strain the Achilles tendon. Additionally, wearing flip flops may make it easier to fall, and the toes may become bruised. It is beneficial to wear flip flops to the pool, beach, and shower areas, but your overall foot health may benefit from limiting the time that your feet spend in flip flops. If you would like more information about the dangers of wearing this type of shoe, please consult with a podiatrist.
Flip-flops are not always the best choice of footwear. If you have any concerns about your feet or ankles, contact Dr. Henry Miller from New Jersey. Our doctor will assist you with all of your foot and ankle needs.
Flip-Flops and Feet
When the weather starts warming up, people enjoy wearing flip-flops. Flip-flops are comfortable, stylish, and easy to slip on and off; they're perfect for any summer beach goer. However, these shoes can cause harm to the feet.
How Can Flip-Flops Affect Me Long-Term?
Are There Injuries Associated with Flip-Flops?
Yes. Since flip-flops are relatively weak and do not provide the same amount of support as sneakers, people who wear flip-flops regularly are more susceptible to injuries. On top of that, the open nature of the shoe makes your feet more prone to other problems, such as cuts and even infections. Common injuries and ailments include:
I like Wearing Flip-Flops. Are There Safe Alternatives?
When buying flip-flops, try to find ones that have sturdy soles and that are made of high-quality materials that will support for your feet. These flip-flops will cost more but will also last longer as a result.
If you have any questions please feel free to contact our office located in Freehold, NJ . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
When the weather heats up, you may want to start wearing flip-flops. However, it has been proven that these are not the ideal shoes in terms of preserving the health of your feet.
Flip flops are known to expose your feet to different types of bacteria and fungal infections. When you wear your flip flops in public, you are exposing them to staphylococcus which is a skin-irritating bacterium. Athlete’s foot is also highly contagious and can be spread when you walk around nearly-barefoot.
Another harmful effect of wearing flip-flops is that they develop blisters on the feet. This is because the thin strap rubs against the skin with each step taken. Unfortunately, when blisters pop, they cause you to be more vulnerable to pathogens you pick up by having your feet exposed.
These shoes may also cause “shooting pains”. If you have flat feet, you need arch support to keep your knees, hips, and back in alignment. If you wear flat shoes, your joints are forced to compensate which can cause injuries throughout the body.
If you constantly wear flip-flops, you should avoid doing so as they can lead to many problems for your feet. If you are experiencing any of these foot issues, you should seek help from a podiatrist right away.
 Research has indicated that falling is a leading cause of injury in older people. Many patients can experience a fear of falling, and this can lead to the inability to perform daily activities. Falling may be caused by several factors, including wearing shoes that do not fit correctly, having poor vision, taking multiple medications, or rushing and walking too quickly. There are effective prevention methods that can be implemented, which may help to prevent falling episodes. These can consist of removing worn rugs from the living environment, and improving lighting in the household. Additionally, it is beneficial to engage in a routine exercise program as this can be helpful in improving overall strength. If you would like more information about how falling can affect the feet, please confer with a podiatrist.
Research has indicated that falling is a leading cause of injury in older people. Many patients can experience a fear of falling, and this can lead to the inability to perform daily activities. Falling may be caused by several factors, including wearing shoes that do not fit correctly, having poor vision, taking multiple medications, or rushing and walking too quickly. There are effective prevention methods that can be implemented, which may help to prevent falling episodes. These can consist of removing worn rugs from the living environment, and improving lighting in the household. Additionally, it is beneficial to engage in a routine exercise program as this can be helpful in improving overall strength. If you would like more information about how falling can affect the feet, please confer with a podiatrist.
Preventing falls among the elderly is very important. If you are older and have fallen or fear that you are prone to falling, consult with Dr. Henry Miller from New Jersey. Our doctor will assess your condition and provide you with quality advice and care.
Every 11 seconds, an elderly American is being treated in an emergency room for a fall related injury. Falls are the leading cause of head and hip injuries for those 65 and older. Due to decreases in strength, balance, senses, and lack of awareness, elderly persons are very susceptible to falling. Thankfully, there are a number of things older persons can do to prevent falls.
How to Prevent Falls
Some effective methods that older persons can do to prevent falls include:
Falling can be a traumatic and embarrassing experience for elderly persons; this can make them less willing to leave the house, and less willing to talk to someone about their fears of falling. Doing such things, however, will increase the likelihood of tripping or losing one’s balance. Knowing the causes of falling and how to prevent them is the best way to mitigate the risk of serious injury.
If you have any questions, please feel free to contact our office located in Freehold, NJ . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Elderly Americans are very susceptible to falls as they get older. Everyone experiences decreases in flexibility, balance, strength, and the senses as they age. This correlates to some eye-opening statistics. 1 in 4 Americans aged 65 and older fall each year. An elderly American is being treated for a fall in an emergency room every 11 seconds. In light of these striking statistics, one can see the importance of taking steps to prevent falls.
Finding an exercise program for the elderly is an excellent way to reduce the likelihood of falls. Look for an exercise program that improves strength and balance. Elderly people who live a more sedentary lifestyle, with little physical activity, are at an increased risk of falling. Wearing well-fitted footwear that provides good foot support and cushion will help prevent falls from poorly fitted shoes. Talking to a podiatrist about your susceptibility to falls and about inspecting your prescriptions will help to avoid any medication that could make falls more likely. Due to a decline in the senses among the elderly, having your eyes and hearing checked is recommended.
Around half of all falls occur in the household. Removing tripping hazards in the home and making it more accommodating to older persons can significantly reduce falls. Some notable household changes include increasing lighting around the house, installing grab bars in the shower and bathroom, and making sure the floor is clear of clutter. Other smart options include installing a shower chair, using rubber-bottomed rugs, and placing railings on both sides of stairwells.
Finally, discuss with a doctor and your family about your fear of falling. This will help to increase awareness among the population on the need for fall prevention. A lack of awareness on the matter, and a downplaying of importance are what increase the risks of falling. Following these tips can help to reduce the risk for yourself and your loved ones.
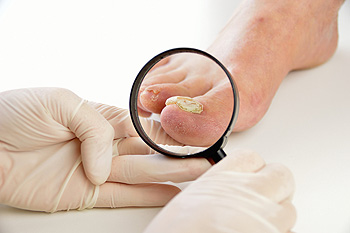 A fungal infection of the toenails is a very common condition that can cause the nails to become thickened, yellowed, or crumbly. This can sometimes lead to pain in the affected toenails. There are a variety of treatments available for fungal nail infections. Currently, a common treatment is an oral antifungal medication. While these medications have a high rate of curing the infection, it can take up to a year before you see visible results, and some people may experience side effects from taking the medication. Topical medications that are applied directly to the nail tend to have less side effects than oral medications, but are typically less effective. Some newer treatments, such as laser therapy, are still being studied, and have shown promising results thus far. If you have toenail fungus, it is recommended that you visit a podiatrist for treatment.
A fungal infection of the toenails is a very common condition that can cause the nails to become thickened, yellowed, or crumbly. This can sometimes lead to pain in the affected toenails. There are a variety of treatments available for fungal nail infections. Currently, a common treatment is an oral antifungal medication. While these medications have a high rate of curing the infection, it can take up to a year before you see visible results, and some people may experience side effects from taking the medication. Topical medications that are applied directly to the nail tend to have less side effects than oral medications, but are typically less effective. Some newer treatments, such as laser therapy, are still being studied, and have shown promising results thus far. If you have toenail fungus, it is recommended that you visit a podiatrist for treatment.
If left untreated, toenail fungus may spread to other toenails, skin, or even fingernails. If you suspect you have toenail fungus it is important to seek treatment right away. For more information about treatment, contact Dr. Henry Miller of New Jersey. Our doctor can provide the care you need to keep you pain-free and on your feet.
Symptoms
Treatment
If self-care strategies and over-the-counter medications does not help your fungus, your podiatrist may give you a prescription drug instead. Even if you find relief from your toenail fungus symptoms, you may experience a repeat infection in the future.
Prevention
In order to prevent getting toenail fungus in the future, you should always make sure to wash your feet with soap and water. After washing, it is important to dry your feet thoroughly especially in between the toes. When trimming your toenails, be sure to trim straight across instead of in a rounded shape. It is crucial not to cover up discolored nails with nail polish because that will prevent your nail from being able to “breathe”.
In some cases, surgical procedure may be needed to remove the toenail fungus. Consult with your podiatrist about the best treatment options for your case of toenail fungus.
If you have any questions, please feel free to contact our office located in Freehold, NJ . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Fungal infection of the toenail, or onychomycosis, typically appears as a gradual change in a toenail’s texture and color that involves brittleness and darkening. The fungal infection itself occurs beneath the surface of the nail. Aside from discoloration, other symptoms include the collection of debris beneath the nail plate, white marks on the nail plate, and a foul odor emanating from the nail. If ignored, the infection can spread into other nails and the skin; in severe cases, it can hinder one’s ability to work or walk.
The toenails are particularly vulnerable to contracting infection in moist environments where people are likely to be walking barefoot, such as around swimming pools, public showers, and locker rooms. Fungal infection may also be more likely to occur in nail beds that have been injured, and sufferers of chronic diseases such as diabetes, circulatory problems, or immunodeficiency conditions are particularly prone to developing fungal nails.
Fungal nails can be primarily prevented by practicing proper hygiene and regularly examining the feet and toes. Carefully washing the feet with soap and water and thoroughly drying the feet afterwards are essential. Other tips include wearing shower shoes in public areas, changing shoes and socks daily, keeping toenails clipped at a short length, wearing breathable shoes that fit properly, wearing moisture-wicking socks, and disinfecting home pedicure tools and instruments used to cut nails.
Fungal nail treatment may vary between patients and the severity of the condition. Your podiatrist may suggest a daily routine of cleansing that spans over a period of time to ease mild infections. Over-the-counter or prescription antifungal agents may also be prescribed, including topical and/or oral medications. Debridement, or the removal of diseased nail matter and debris, may also be performed. In more severe cases, surgical treatment may be needed. In some instances, the temporary removal of the fungal nail allows for the direct application of a topical antifungal to the nail bed. In other cases, a chronically painful fungal nail that has not responded to other treatments may be permanently removed; this allows the infection to be cured and avoids the growth of a deformed nail.
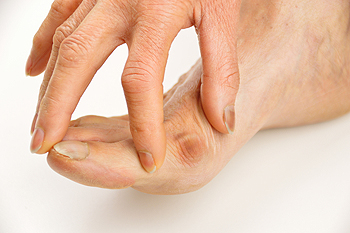 The medical condition that is referred to as arthritis may contribute to the development of bunions. Additionally, bunions can occur due to genetic factors, or from wearing shoes that do not have enough room for the toes to move freely in. Bunions are defined as bony growths that form on the side of the big toe and can cause pain and discomfort. Mild relief may be found when a protective pad is worn over the bunion, and larger shoes may need to be purchased. An X-ray may be performed to determine the severity of the bunion, and if it is large, and affects daily activities, surgery may be necessary for permanent removal. If you have developed a bunion, please consult with a podiatrist who can determine what the best course of treatment is for you.
The medical condition that is referred to as arthritis may contribute to the development of bunions. Additionally, bunions can occur due to genetic factors, or from wearing shoes that do not have enough room for the toes to move freely in. Bunions are defined as bony growths that form on the side of the big toe and can cause pain and discomfort. Mild relief may be found when a protective pad is worn over the bunion, and larger shoes may need to be purchased. An X-ray may be performed to determine the severity of the bunion, and if it is large, and affects daily activities, surgery may be necessary for permanent removal. If you have developed a bunion, please consult with a podiatrist who can determine what the best course of treatment is for you.
If you are suffering from bunions, contact Dr. Henry Miller of New Jersey. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is a Bunion?
A bunion is formed of swollen tissue or an enlargement of boney growth, usually located at the base joint of the toe that connects to the foot. The swelling occurs due to the bones in the big toe shifting inward, which impacts the other toes of the foot. This causes the area around the base of the big toe to become inflamed and painful.
Why Do Bunions Form?
Genetics – Susceptibility to bunions are often hereditary
Stress on the feet – Poorly fitted and uncomfortable footwear that places stress on feet, such as heels, can worsen existing bunions
How Are Bunions Diagnosed?
Doctors often perform two tests – blood tests and x-rays – when trying to diagnose bunions, especially in the early stages of development. Blood tests help determine if the foot pain is being caused by something else, such as arthritis, while x-rays provide a clear picture of your bone structure to your doctor.
How Are Bunions Treated?
If you have any questions, please feel free to contact our office located in Freehold, NJ . We offer the newest diagnostic and treatment technologies for all your foot care needs.
A bunion is an enlargement of the base joint of the toe that connects to the foot, often formed from a bony growth or a patch of swollen tissues. It is caused by the inward shifting of the bones in the big toe, toward the other toes of the foot. This shift can cause a serious amount of pain and discomfort. The area around the big toe can become inflamed, red, and painful.
Bunions are most commonly formed in people who are already genetically predisposed to them or other kinds of bone displacements. Existing bunions can be worsened by wearing improperly fitting shoes. Trying to cram your feet into high heels or running or walking in a way that causes too much stress on the feet can exacerbate bunion development. High heels not only push the big toe inward, but shift one's body weight and center of gravity towards the edge of the feet and toes, expediting bone displacement.
A podiatrist knowledgeable in foot structure and biomechanics will be able to quickly diagnose bunions. Bunions must be distinguished from gout or arthritic conditions, so blood tests may be necessary. The podiatrist may order a radiological exam to provide an image of the bone structure. If the x-ray demonstrates an enlargement of the joint near the base of the toe and a shifting toward the smaller toes, this is indicative of a bunion.
Wearing wider shoes can reduce pressure on the bunion and minimize pain, and high heeled shoes should be eliminated for a period of time. This may be enough to eliminate the pain associated with bunions; however, if pain persists, anti-inflammatory drugs may be prescribed. Severe pain may require an injection of steroids near the bunion. Orthotics for shoes may be prescribed which, by altering the pressure on the foot, can be helpful in reducing pain. These do not correct the problem; but by eliminating the pain, they can provide relief.
For cases that do not respond to these methods of treatment, surgery can be done to reposition the toe. A surgeon may do this by taking out a section of bone or by rearranging the ligaments and tendons in the toe to help keep it properly aligned. It may be necessary even after surgery to wear more comfortable shoes that avoid placing pressure on the toe, as the big toe may move back to its former orientation toward the smaller toes.